What Is Lymphedemea?
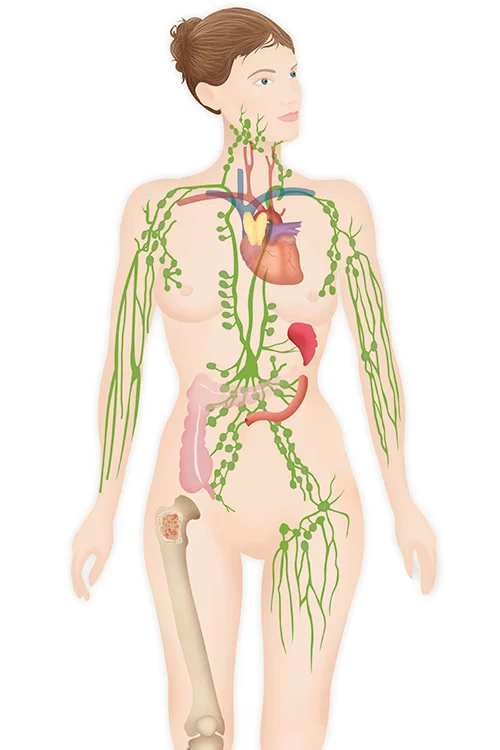
Lymphedema is a chronic, progressive disease characterized by swelling, fat deposition, and fibrosis in one or multiple extremities. It results from dysfunction or disruption to the lymphatic system. The lymphatic system is responsible for transporting fluid through our tissues, and it also filters the fluid for any bacteria or cancer cells and alerts the immune system to fight them.
There are two types of lymphedema. Primary lymphedema is often inherited or congenital. Secondary lymphedema is an acquired condition that is the result of damage to the lymphatic system. In the Unites States, the most common cause of lymphedema is secondary to surgery such as lymph node removal in cancer patients, which is often worsened by radiation therapy. The risk of developing lymphedema can be as high as 35% in certain cases after lymph node dissection.